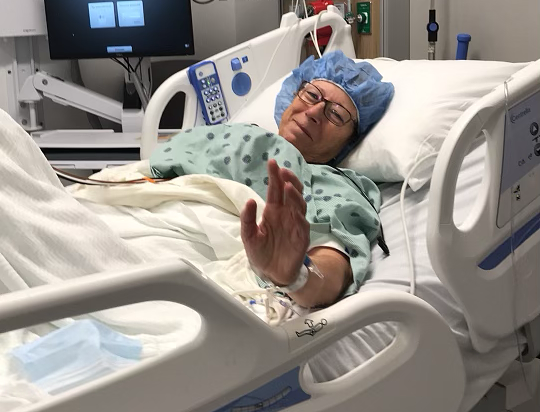
It was late October 2023, and Matt Wingler was working his regular shift as Deputy Chief of Owen Valley Fire Territory in Spencer.

He and his team were performing routine hose testing when the water pump abruptly ruptured, sending a large hose and metal coupling into his leg.
“I immediately got away from the truck,” says Wingler. “However, I couldn’t move my right leg without severe pain.”
His leg immediately started swelling to a concerning size, so his crew took him to a local hospital that confirmed severe soft tissue trauma but no fracture to the bone.
“I was discharged from the ER with no follow-up plan or pain management,” says Wingler. “After getting home, I knew it was worse than they thought since the pressure was building in my leg.”
He called his IU Health Primary Care provider, Margaret Pejeau, NP, and she and her team helped him manage the pain, but the continued swelling in his leg tore into an open wound.
That’s when Pejeau referred him to IU Health Wound Care.
“After the referral, things went so much better, and I will forever be thankful for the Bloomington wound care team,” he says.
“We have an excellent team that provides emotional support and detailed explanations on how wound care works,” says Wauneta Armstrong, FNP-C, who was part of Wingler’s Wound Care team. “The team here goes above and beyond every day to make sure our patients are comfortable.”
Wingler was sent for a CT scan to evaluate the severity after his first Wound Care appointment and the nurse practitioner called him after her shift to share the results so he’d have peace of mind over the weekend.
Within a month of weekly follow-up care by the IU Health Wound Care team, the open wound finally healed with no further complications.
Armstrong credits her team’s educational efforts on the importance of rest and wound care for the successful healing of this particular injury.
“I would just like to share my appreciation for the incredible, compassionate service provided by the IU Team,” says Wingler. “Every member of the IU Health team really showed compassion and a shared goal of healing my leg quickly so I could return to full duty.”